The SoR has responded to news published by The Guardiannewspaper revealing the government is planning to cut millions of pounds in funding for AI in radiotherapy.
On Monday (31 March), The Guardian published an exclusive news story which revealed that funding for AI contouring in radiotherapy would be cut "due to a need to further prioritise limited investment."
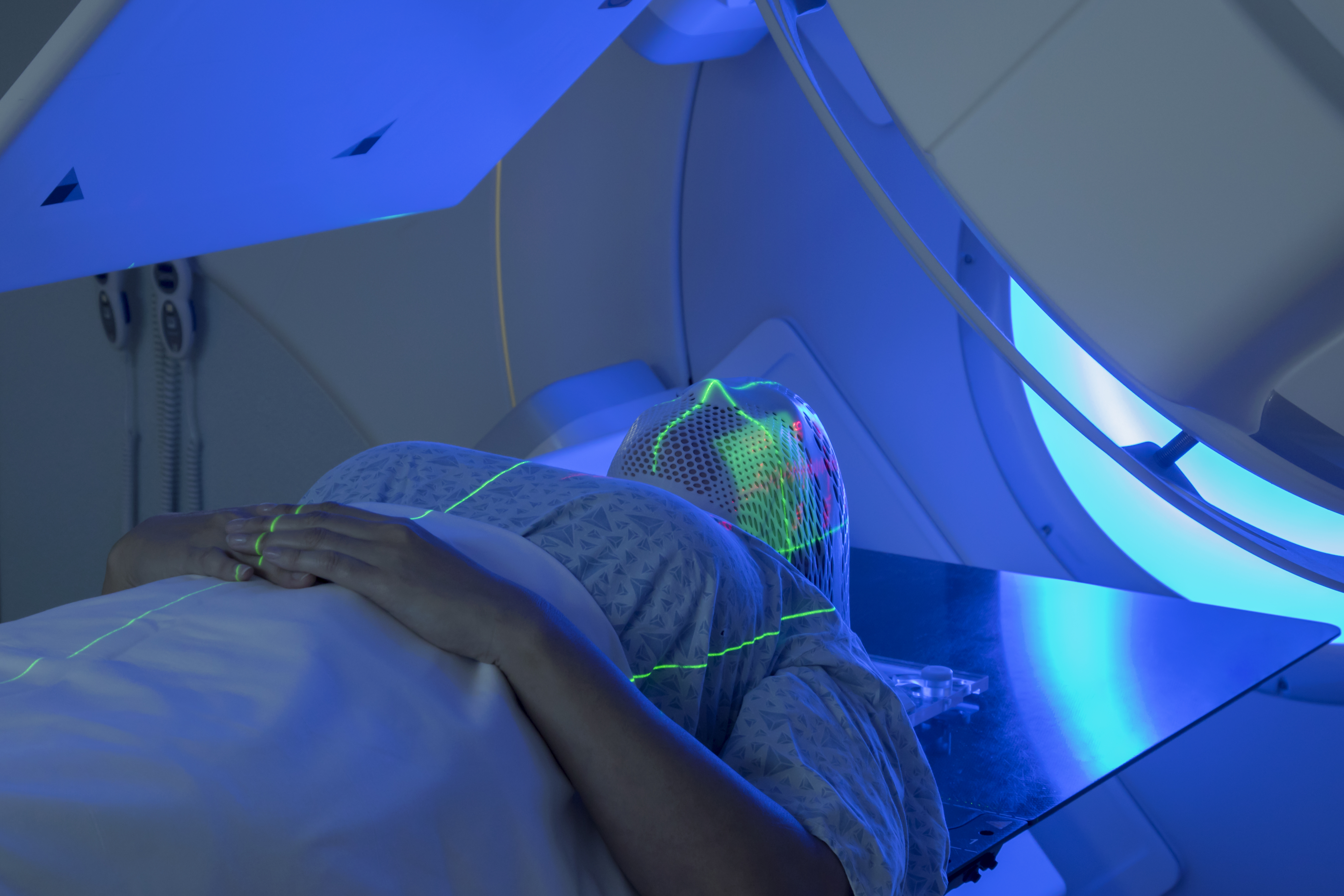
Radiotherapy contouring is a process that ensures radiation targets the cancer while minimising damage to healthy tissues and organs. While this process can take up to two hours when done manually, AI auto-contouring takes less than five minutes and costs around £10-£15 per patient.
Research has demonstrated that such technology could reduce waiting times and help to address staff shortages – but only if there is availability across the whole patient pathway, which is not always the case.
'The transformative potential of AI'
In May 2024, the Conservative government announced £15.5m over three years to fund AI auto-contouring for all hospitals providing radiotherapy. The 51 trusts offering radiotherapy continued installing the cloud-based technology following the general election in the belief the funding was secured.
However, an email seen by The Guardian in February has revealed Nicola McCulloch, the deputy director of specialised commissioning at NHS England, said the funding had been cancelled “due to a need to further prioritise limited investment”, and there would be no centrally funded programme to support implementation of the technology.
Spencer Goodman, professional officer for radiotherapy at the SoR, said: “Radiographers have long recognised and embraced the transformative potential of AI and other technological advancements in improving the efficiency and accuracy of patient care.
“Withdrawing funding for AI technologies that assist in vital tasks, such as accurately defining radiation fields in radiotherapy, represents a concerning step backward."
The Royal College of Radiologists (RCR) has published clinical documentation on auto-contouring in radiotherapy, outlining the benefits artificial intelligence can bring to the process.
'A significant contribution'
Spencer added: “AI is designed to complement, not replace, the expertise of skilled clinicians who specialise in image interpretation, radiation safety, and the optimal application of radiotherapy. In an environment where there is already a shortage of these experts, AI that has been proven to aid in the process can make a significant contribution.
“It can help streamline workflows, improve accuracy, and enable patients to receive faster, more efficient treatment. The strategic integration of AI into clinical practice is key to ensuring that both healthcare providers and patients benefit from the best that technology and human expertise have to offer.”
While AI is one way in which the persistent issues facing the NHS could be addressed, Mr Goodman emphasised that it was not the only way.
“It is important to review the whole care pathway,” he added, “As a siloed approach to funding specific points in care will not provide the ability to improve access to treatment.”
'Slowing down the work'
Tracy O’Regan, professional officer for clinical imaging and research at the SoR, shared Mr Goodman’s concern.
She said: “This is a major setback to plans to further reduce waits for radiotherapy treatment. AI assisted digital systems have the potential to allow the teams who work in radiotherapy departments, including Therapeutic Radiographers, to speed up the contouring process and improve patient care and outcomes. Waiting lists for crucial cancer care are not meeting the targets set, or the standards that we want to meet, for patients.
“At what is a very stressful time for people who are diagnosed with cancer, we must further develop the technology that we use to treat people and ensure that staff have access to all of the technological resources they can use to do that, including AI assisted auto-contouring methods. Withdrawing access to the funding that will enable a full evaluation of those software systems in real-world settings is effectively blocking or slowing down that work.”
She added that the Health and Care Professions Council (HCPC) has outlined its expectation on the standards of proficiency for radiographers around using AI, machine learning and deep learning models, as both Diagnostic and Therapeutic Radiographers and sonographers are using AI systems for a variety of reasons across the breadth of their practice.
The Society of Radiographers supports SoR members with advice, guidance, education, and research with respect to AI. The SoR's new three-year strategic framework, Vision for Our Profession, reflects the society’s ambition to help harness technology further, to meet patients’ needs quickly and with increased accuracy.
Immediate and urgent funding
The RCR’s UK Radiotherapy Board Policy briefing said that four key areas required immediate and urgent funding, to address the crisis afflicting healthcare in the UK:
- Workforce Shortages: Immediate funding is needed to unlock existing workforce vacancies and ensure that staffing levels meet demand.
- Recruitment & Retention: Increased investment is crucial to attract, train, and retain skilled professionals, ensuring long-term sustainability and quality of service.
- Clinical Capacity to Embed Research & Innovation: Enhanced funding will support the continued integration of research and innovation into clinical practice, improving patient care and advancing the field of radiotherapy.
- Pathway Redesign: Additional resources are essential to redesign patient pathways, improving efficiency and ensuring timely access to treatment
Additionally, the SoR is currently gathering responses for a submission to the Department of Health and Social Care Cancer Plan consultation, which will include the Clinical Imaging requirements and pathway for these patients.
Radiographers and the general public can also contribute to this consultation online at the link above.
(Image: Woman undergoing radiotherapy, by Mark Kostich via Getty/images)
